Remdesivir no Cure for the Covid and Oxygen does not need routine application
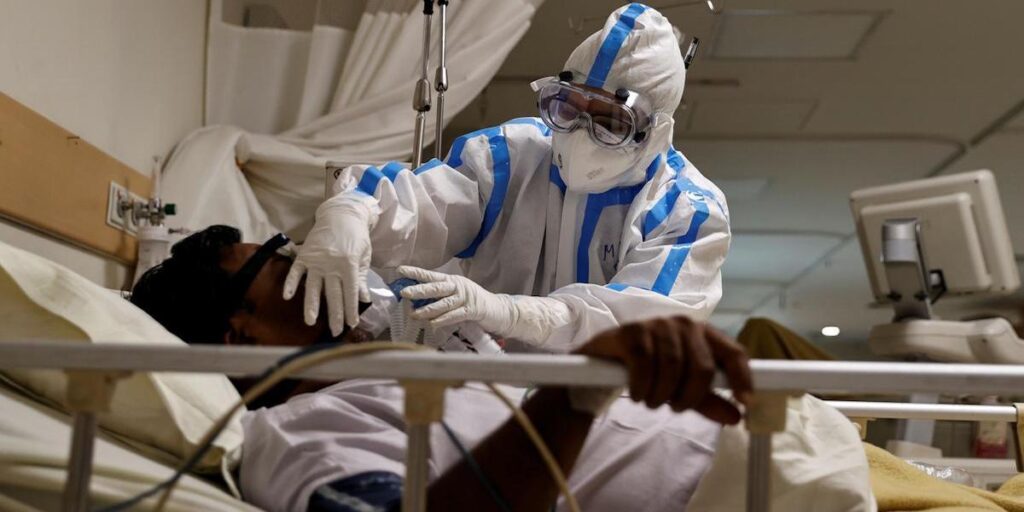
Through a graded, pre-emptive and pro-active approach, Government of India is taking several steps along with the States/UTs under a ‘whole of government’ approach for prevention, containment and management of the recent surge in COVID-19 cases. These are also being regularly reviewed and monitored at the highest level.
The Department for Promotion of Industry and Internal Trade (DPIIT), the central government department under the Ministry of Commerce and Industry, in consultation with all stakeholders, has issued a supply mapping plan for 12 high burden states till 30th April. The Home Ministry’s advisory on unhindered movement of oxygen across states, the installation of 162 PSA Oxygen plants (154.19 MT capacity) in 32 States/UTs from PM-CARES fund, Operationalization of the IT application, ‘Medsupply’ which tracks site readiness, plant delivery, installation & commissioning, augmentation of Remdesivir production to around 74.10 lakh vials/month (May)from 27-29 lakh vials/month (Jan-Feb), Prohibition on the export of Remdesivir API and formulations by the DGFT, Stringent actions on black marketing and hoarding of the drug are some of the decisions taken to ease the difficulty of those affected by COVID.
There has been an unprecendented surge of daily new COVID cases across the country, with the resultant increase in the consumption of some drugs such as Remdesivir. Clinical management of COVID patients with severe symptoms in hospitals has also lead to a high consumption of oxygen. The Union Government has taken various steps to boost the supply of oxygen in the hospitals across the country, in the recent days.
Three prominent doctors of the country, Prof (Dr) Randeep Guleria, Director, AIIMS, Dr. Devi Shetty, Chairman, Narayana Health and Dr. Naresh Trehan, Chairman, Medanta Hospital, addressed various issues being related to the rational utilization of Remdesivir, included under the category of Investigational therapy under the National Treatment Protocol of the Health Ministry, and use of Oxygen for treatment of COVID patients in hospitals.
Vaccine
Dr. Guleria exalted the vaccine as the key to beat the gloom that is usually associated with COVID: although it may not prevent us from getting the infection, the vaccine prevents us from getting the disease in the form of severe illness. He said that it was important to understand that even after the vaccination, we may become infected with COVID which makes it important to continue to wear a mask even after getting vaccinated.
Oxygen
Dr. Guleria reassured that healthy individuals with oxygen saturation in the range 93-94% do not need to take high flow oxygen just to maintain their saturation at 98-99%. Even those with oxygen saturation less than 94 need close monitoring (oxygen being optional).
“Oxygen is a treatment, it’s like a drug” he stated to drive home the point that taking oxygen intermittently is an absolute waste of oxygen. There is no data that shows that this will be of any help to the patients and is therefore ill-advised.
Dr. Trehan echoed his observations and observed that the country has enough oxygen if we try to use it judiciously. He requested the audience not to use Oxygen as a “security blanket”. Waste of oxygen will only lead to depriving someone who needs it.
Dr. Shetty noted that a saturation above 94% is no problem. A doctor may be consulted if it dips after exercise/effortful work.
Remdesivir
All the doctors unanimously requested the audience to desist from seeing Remdesivir as a wonder drug. Most of the active cases who are in home isolation or in the hospital don’t actually need any specific treatment. Only a small percentage require Remdesivir.
They were of the view that as a country, if we work together, use oxygen and Remdesivir judiciously, then, there will be no shortage anywhere. In terms of the number of people who need oxygen and oxygen supply, we are well balanced, they noted.
Dr. Trehan agreed and added that his hospital has now made a protocol that Remdesivir is to be given not to everyone who tests positive. It is to be given only after doctors look at test results, symptoms, comorbidities of a patient. Remdesivir isn’t a ‘Ram-ban’, it only decreases viral load in people who need it.
General Issues
Dr. Guleria said that when it comes to COVID, more than 85% of people will recover without any specific treatment in the form of Remdesivir etc. Most will have symptoms like common cold, sore throat etc and over 5-7 days, they will recover with symptomatic treatment. Only 15% may go to moderate phase of the disease.
He advised against being in groups irrespective of somebody being infected and observed that Cross ventilation reduces the risk of infection in closed places.
Dr Trehan echoed the sentiment that since less percentage of people require hospitalization, the hospital beds should be utilized judiciously & with responsibility which rests on all of us.
Dr Shetty advised to see a doctor and get their opinion if one is positive. He further advised to not panic if the report is positive as the problem can be solved provided one gets the medical help at an early stage & follow doctor’s instructions.
There is a possibility that patient may be asymptomatic prompting the doctors to tell them to stay at home, isolate themselves, wear a mask and check their oxygen saturation every 6 hours. He also suggested to get tested if anyone have any symptom like body ache, cold, cough, indigestion, vomiting since that is the basis of any further treatment.
It may be noted here that Dr Nishit Sud of Anaesthetics/Critical Care, NHS London, has written the following (London, incidentally, had also undergone a, intense second Covid attack) :
ENGLAND LESSONS FOR INDIA ON VIRUS
Lessons from the second wave. India today seems to be in the exact same situation that the UK was in mid december. First an exponential number of people testing Covid positive followed a week later by an exponential increase in number of hospitalizations followed 2 weeks later by an exponential increase in Covid deaths. Here are some of the lessons learnt
1. 99% of Covid positive recover on their own. The only things needed for them are oxygen level monitoring to make sure sats are >93, paracetamol (Crocin or Dolo) for fever and bodyache and home isolation to make sure they do not pass it on to others. There is no need or benefit in giving plasma, remdesivir, ivermectin, hydroxychloroquine, antibiotics or even steroids, blood thinners or toclizumab to these 99%. There is NO need for hospitalization as long as oxygen levels are above 93%.
2. Covid is an illness that affects a lot of people at the same time, however it is how severely it affects the 1% who are unlucky enough to have severe covid which makes it the dreaded illness it is. All our medical resources (hospital beds, oxygen cylinders etc) need to be saved for these severely affected 1% and not the 99% with mild illness irrespective of wealth, contacts, influence etc.
3. For the 1% that have severe illness the only medications that have been found to have significant benefit are steroids and blood thinners. Toclizumab also has been found to have benefit (only 4%) and should be given whenever available. Remdesivir has very minimal benefit (no mortality benefit at all) and should be given if available however the patient does not loose much if not given . However it will be wrong to call either of them (toclizumab/remdesevir) life saving in Covid.
4. Plasma has been extensively studied and found to be of no benefit. This is after painstaking analysis of 11,000 patients given plasma vs 11,000 not given plasma. It should NOT be given. It uses up a significant amount of resources with no benefit.
5. Hydroxychloroquine/Ivermecin. No serious medical organisation is the world found any benefit in giving them and should not be given. However they are cheap and relatively harmless .
6. Oxygen shortage – Many hospitals in the UK had to stop admitting patients due to running out of oxygen for short periods of time. We only need to give enough oxygen for levels to be above 93 to 94 . There is often a tendency to turn oxygen flows to the highest levels possible. This has to be avoided.
7. Vaccine. In London before the vaccine all our ICUs were full, all theatre recoveries were full, all cardiac HDUs etc were full of intubated covid patients and we were transferring intubated covid patients to as far as Scotland, Bristol etc in helicopters to relieve ICU capacity in London. After the vaccine we have hardly any hospital admissions and almost nil new ICU admissions. However this could also have been due to the serious nature of the lockdown.
8. Rationing of resources. In the UK every patient who needed a hospital bed got one and every patient who was suitable for an ICU bed got one. This was only possible as there were strict criteria for hospital admission which meant that the 99% of Covid positive who do not need oxygen were not hospitalised. This needs to be done strictly in India as well.
9. Once someone has tested covid positive there is no need to get retested to see if they are still covid positive. This unnecessary re-testing results in wastage of testing resources. Once 2 weeks of home isolation following date of onset of symptoms is complete a person is considered covid negative and non infectious.